GP’s, Nutritionists, and Dietitians now have a real option for treating patients with IBS.
THE 28-DAY GUT DYSBIOSIS PROGRAM
- Advised by a Gastroenterologist
- Relieves the symptoms & treats the cause of IBS
- Rebalances the microbiome
- 100% natural
An effective plan for IBS
Traditional medicine has struggled to manage patients with chronic irritable bowel syndrome (IBS) for decades. The prevailing dogma being the cause of IBS is largely unknown and there is no effective treatment.
BUT, medical research* has defined IBS as a state of bacterial imbalance in the gut microbiome called dysbiosis and has shown that correction of this imbalance is a valid way to treat IBS.
The IBS Doctor 28-Day Program is made up of a specific combination of diet, supplements, probiotics, and prebiotics that when combined together help provide effective relief of the symptoms of IBS.
These symptoms may include:
- Abdominal pain, cramps, or discomfort
- Diarrhoea, constipation, or both
- Bloating and wind
- Poor digestion
- Low mood, brain fog or fatigue
If you have any questions, please contact us.
*Lee et al. Intestinal microbiota in pathophysiology and management of IBS. World J Gastroenterol 2014 July 21; 20(27): 8886-8897.

If you’d like a patient to do the program, simply ask your them to order it from our store.
Depending on symptoms, patients will follow either a Diarrhoea based plan, or a Constipation based plan.
For convenience, the supplements have been pre-packed into Webster Packs in correct doses. The program is broken into two phases.
Phase 1 (Days 1-14)
Cleanse

In Phase 1, we cleanse away the bad bacteria and the biofilms that protect them with a course of natural cleansing supplements and easy-to-follow dietary advice. These bacteria make many toxins that interfere with digestion, bowel function and irritate the gut nerves.
Phase 1 includes:
- Natural Dysbiosis Cleansing Supplements
- Natural Biofilm Cleansing Supplements
- Natural Gut Immune Boosting Supplements
- 1 x cannister of Immunity Tea
- Phase 1 – Cleansing Low FODMAP Diet
Phase 2 (Days 15-28)
Reload

In Phase 2, we reload the gut with good healthy bacteria through a regime of natural probiotic and prebiotic supplements and our Gut Reload Diet. These bacteria make a multitude of nutrients that improve digestion, calm the gut nervous system and restore normal bowel movements.
Phase 2 includes:
- Natural Prebiotic Supplements to restore bowel function
- Natural Probiotic Supplements to restore healthy gut bacteria
- Natural Nutraceuticals to repair the gut lining
- 1 x cannister of Detox Tea
- 1 x tin of Organic Chicken Bone Broth – Garden Herb
- Phase 2 - Gut Reload Probiotic Diet.
Phase 3
Maintenance
Once the patient has completed the program, it’s important for them to maintain their gut microbiome and general health with daily probiotic and prebiotic supplements.
The maintenance program is essentials for ongoing success. If it’s not followed, patients will go backwards, and symptoms may return.
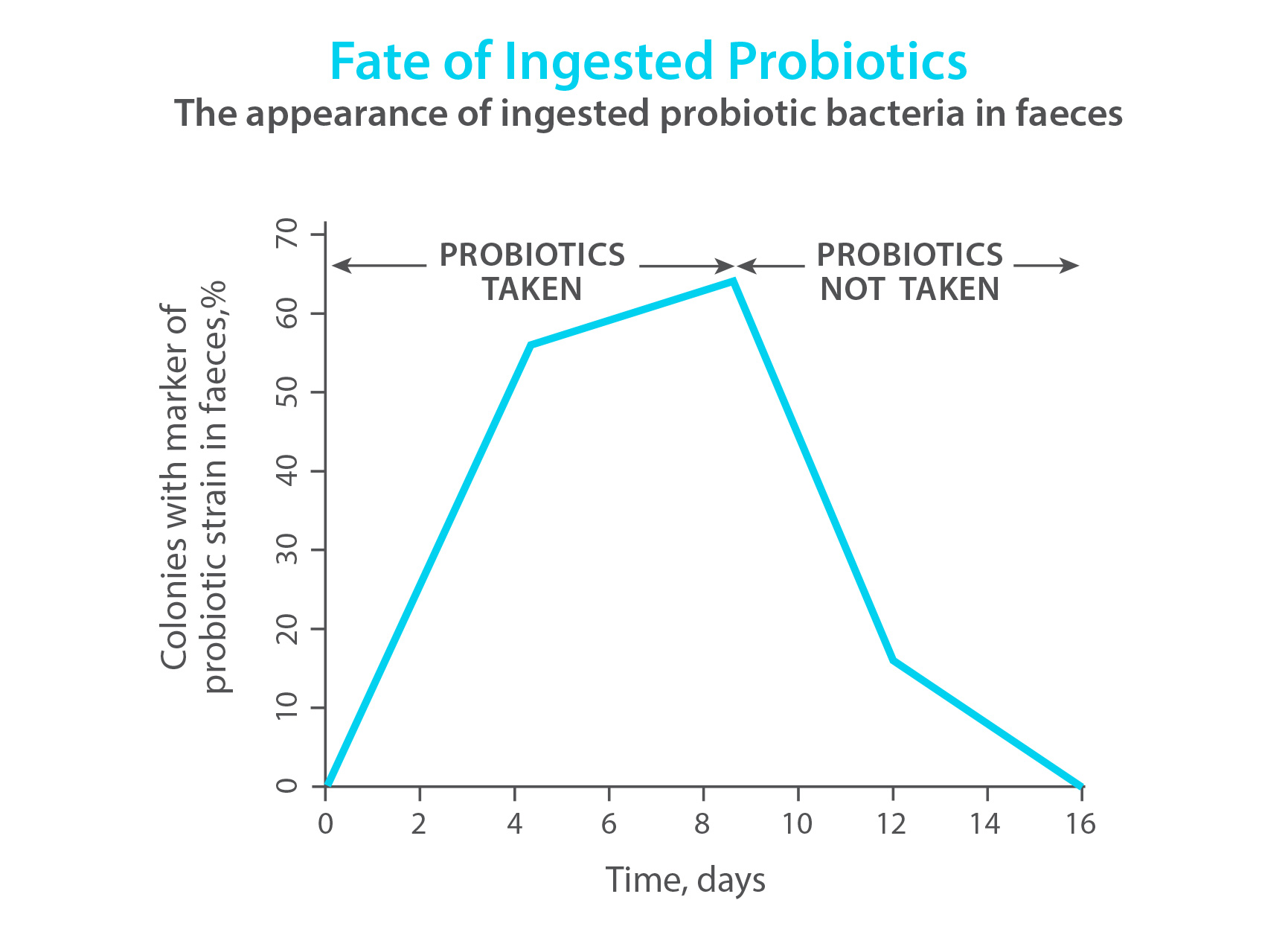
Probiotics don't live in the gut forever; they disappear within 2 weeks of stopping them. So only through regular supplementation can you keep the gut healthy and functioning properly.
The benefits of good bacteria
Good bacteria make nutrients for us like:
- B group vitamins
- Vitamin K
- Amino Acids
- Short chain fatty acids
- CoQ10 for energy production
- Glucosamines for joints
- Serotonin for mood
These nutrients:
- Improve digestion of food
- Calm the gut nervous system
- Restore normal bowel movements
- Reduce sweet food cravings
- Control body weight
- Improve mood and concentration
- Clear the skin
- Boost energy
They also keep us healthy by:
- Maintaining good digestion
- Regulate bowel movement
- Bind carcinogens
- Modulate appetite and body fat
- Stabilize mood and stress
- Protect us against gastroenteritis
- Boost the immune system
- Teach us to tolerate foods
Dietary advice
There is no diet that will cure IBS. However, the right dietary advice combined with prebiotic and probiotic supplements can achieve desired outcomes. Our tailored diet has been designed to suit your patient’s lifestyle and is intended as a guide only. They can take out of it, what they want. All our dietary advice has been developed in consultation with a qualified Dietitian.
The effects of bad bacteria
Bad dysbiotic bacteria stops production of all the good nutrients listed here. They also make toxins like LPS, ETX, aldeh, lactate, amine and H2S which causes the intestinal barrier to become ‘too permeable’ also known as Leaky Gut and triggers inflammation.
This causes IBS symptoms like:
- Abdominal pain
- Cramps
- Diarrhoea
- Constipation
- Fatigue
- Low mood
- Brain fog
- Skin rashes
- Joint pains
- Sweet food cravings
- Weight gain
These toxins also:
- Inhibit proper digestion of food
- Irritate the gut nervous system
- Disrupt the normal bowel movements.
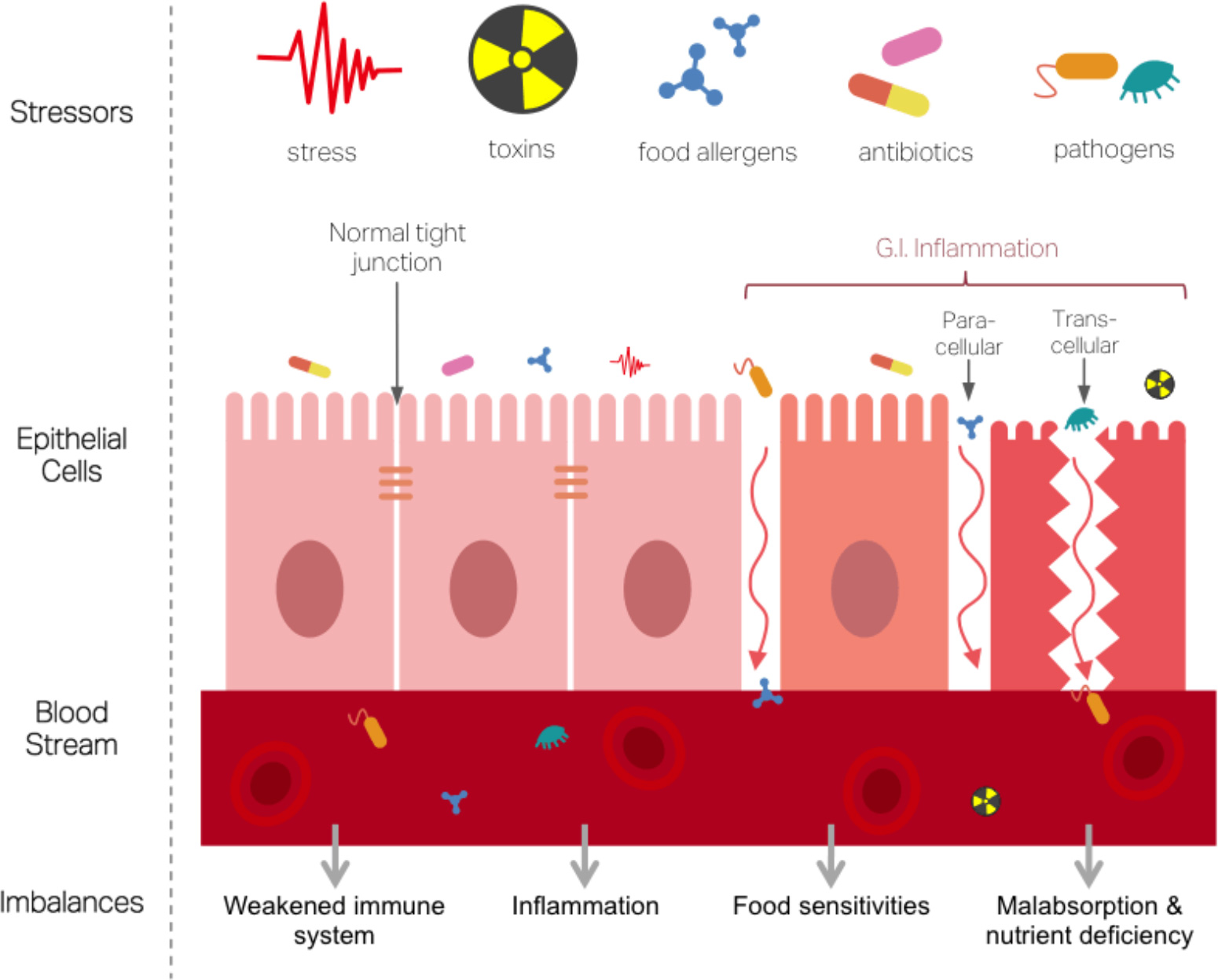
Dysbiotic bacteria causes the intestinal barrier to become ‘too permeable’ and triggers inflammation.
Gut Microbiome Profiling
Quantitative single-phase PCR gut bacterial gene analysis measures the levels of opportunistic pathogens and probiotics from a patient’s stool sample. An advanced technique called cycle threshold amplification is used to quote actual levels of good and bad bacteria within the whole gut family.
A Complete Microbiome Test Kit will be sent to the patient in the mail by our partners at Nutripath Laboratories. This comprehensive test identifies the various strains of bacteria in the patient’s microbiome and highlights specific bacterial imbalances which may be contributing to their symptoms. Gut Microbiome Profiling is in addition to the IBS Doctor program and is supplied at additional cost. Patients are not required to do the Complete Microbiome Test to do the program.
Why we treat the Microbiome
There is a delicate balance of good vs bad bacteria living in our gut. We’re frequently faced with an overgrowth of bad bacteria or undergrowth of good bacteria as well as infection with pathogenic or disease-inducing microbes. The process of imbalance between good vs bad microbes is well recognised and known as dysbiosis.
When the gut microbiome becomes unbalanced, and an unhealthy diet predominates, the density of immune and sensory cells can become the gut’s Achilles heel, generating significant inflammation, pain and systemic dysfunction that can manifest as inflammatory bowel disease or IBS. Dysbiosis is a state of living with intestinal flora that has harmful effects. It can be described as being due to either putrefaction, fermentation, deficiency, or sensitization.
Imbalance in the intestinal microbiome has been associated with bowel inflammation.* Intestinal microbiota play a substantial role in irritable bowel syndrome (IBS). The microbiota contribute directly to the symptoms of IBS, and altered composition and metabolic activity of the microbiota caused by stress or other psychological disturbances indirectly activate mucosal immunity and inflammation, increase epithelial permeability, and reduce barrier function, thereby activating the sensory-motor dysfunction responsible for a variety of symptoms of patients with IBS.
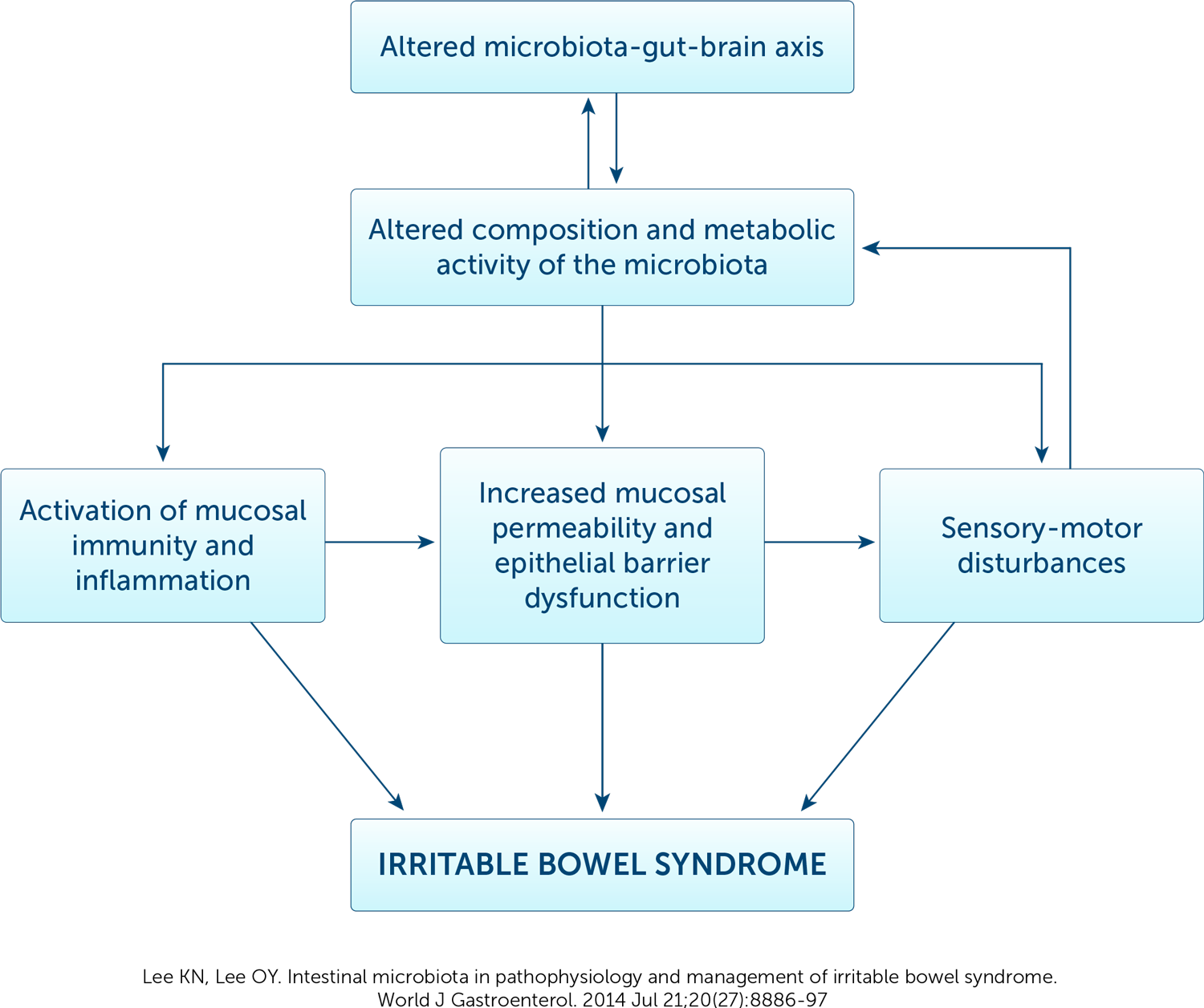
Many studies have repeatedly confirmed the presence of dysbiosis in ulcerative colitis and Crohn’s disease as well as functional gut disorders such as Constipation Predominant-IBS and Diarrhoea Predominant-IBS. Interestingly, the same gut dysbiotic pattern has been established in a host of other conditions such as CFS, autism, Myalgic encephalomyelitis. Many IBS sufferers also complain of milder cognitive symptoms as part of their problem and all patients with CFS etc complain of IBS symptoms. There appears to be an inextricable link between the integrity of the gut mucosal barrier and microbiome with that of both gut and brain function. The first critical step in controlling irritable bowel is to eradicate the overgrowth of bad bacteria in the gut. Without this critical first step, other therapies are unlikely to have any lasting benefit.
Reconstituting a healthy gut microbiome is essential to achieving freedom from IBS. When your gut microbiome is healthy, it can carry out its job without trying to express itself and make one’s life miserable. We are trying to engineer the evolution of our gut microbiome to improve our health, wellbeing, digestion, nutritional state, brain function and mood all of which equals no more suffering from IBS.
*[1] Marteau, Philippe (2009). “Bacterial Flora in Inflammatory Bowel Disease”. Digestive Diseases 27: 99–103. Lepage, P.. (23 April 2012). “A metagenomic insight into our gut’s microbiome”. Gut 62 (1): 146–58.</small
Lactobacillus Bacteria. A good probiotic bacteria.
